Does Human Growth Hormone (HGH) Increase Testosterone?
Does human growth hormone increase testosterone? This is a common point of confusion. Put another way: does HGH actually boost testosterone levels in any meaningful way?
People often notice that HGH is linked with recovery, body composition, and energy – many of the same areas they associate with testosterone. Because the two hormones can influence similar outcomes, HGH is sometimes mistakenly treated as a shortcut for raising testosterone itself. In reality, they work through different pathways, are evaluated differently in the clinic, and are used for different medical reasons.
Now, you’ll see what each hormone actually does, how clinicians usually approach testing and treatment decisions, and why relying on HGH to “fix” low testosterone can lead you away from the real problem – and the right plan.
How HGH and Testosterone Work in the Body
HGH is secreted by the pituitary gland, and it is secreted in pulses; most of this is done during sleep. In adults, it helps in the repair of tissue and has an effect on metabolism. Physicians look at the markers like IGF-1 and the factors like sleep, diet, exercise, medications, and medical history that influence the condition.
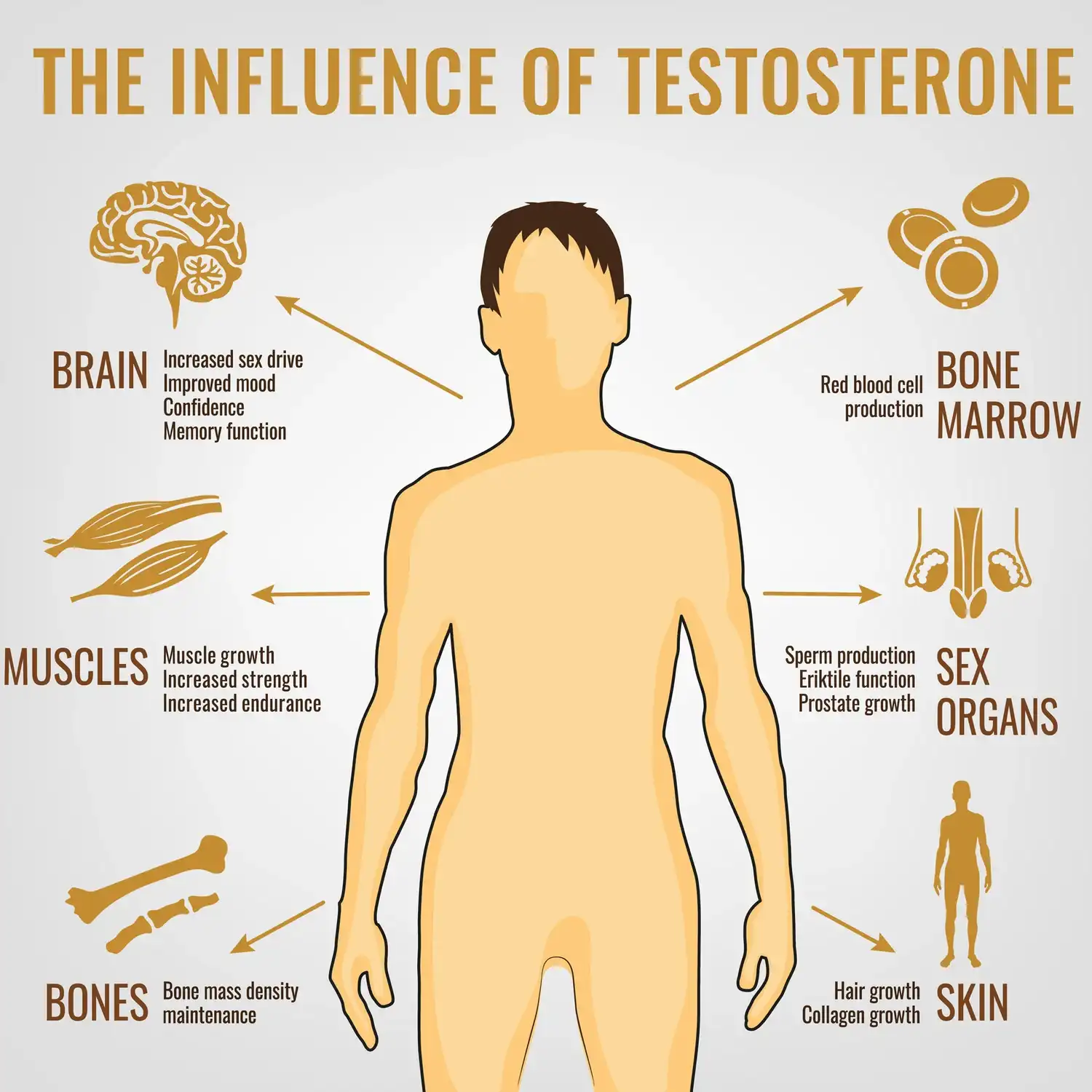
Testosterone is an androgen hormone primarily secreted by the testes and, to a lesser degree, the adrenal glands. The hormone is essential for sexual function, mood, production of red blood cells, bone strength, and muscle preservation. The rate of the brain–ovaries loop regulates its levels, and so changes in sleep, stress, weight, or a whole range of medications can appear as both symptoms and lab values.
So, does hgh affect testosterone? In short, HGH and testosterone can both contribute to similar outcomes – recovery and body composition, to name two – however, it does so through two different biological pathways.
Does HGH Affect Testosterone Levels Directly?
Generally, any relationship between HGH and testosterone, if noticeable at all, tends to be indirect only. HGH is not made into testosterone, and in fact, it doesn’t do what testosterone does in the human body. Does HGH affect testosterone levels? Indirectly. It usually points to the shared basics that shape many hormone rhythms:
- sleep consistency and sleep quality;
- training volume matched to recovery;
- stress load over weeks and months;
- metabolic health, including weight trends and nutrition.
When those improve, people often feel better. Sometimes lab values look better, too. That’s why clinicians focus on repeat testing done under similar conditions, not a single result taken during a rough week. Testosterone can vary depending on sleep debt, illness, hard training, and even the time of day.
Does HGH Increase Testosterone or Just Support Hormonal Balance?
People often get confused when they ask does HGH increase testosterone. Some people believe that they perform better, have improved moods, or react faster when they’re on testosterone. Another way of putting it is: does HGH boost testosterone levels in any meaningful way? The truth is, the questions are actually two distinct ones:
- Are symptoms improving?
- Are hormone levels changing in a consistent, measurable way?
This point is frequently misunderstood. Because the two hormones can influence similar outcomes, HGH is sometimes mistakenly treated as a shortcut for raising testosterone itself. In reality, they work through different pathways, are evaluated differently in the clinic, and are used for different medical reasons.
The two hormones can rise in conjunction with each other, but it is by no means guaranteed. Good sleep and maintaining stable cortisol levels are beneficial for overall hormone health, but should not be seen as a replacement for treating a testosterone deficiency, though.
HGH for Low Testosterone – Why This Approach Is Misleading
Using HGH for low testosterone instead of testosterone replacement therapy (TRT) is a clinical error. Growth hormone and testosterone act via different mechanisms, have different indications for use, and are followed up by different lab markers. Official medical guidelines limit the use of HGH only to growth hormone deficiency cases, not as a method to circumvent hypogonadism.
Depending on HGH in the absence of real TRT can postpone the accurate diagnosis of low testosterone, hide the roots of the problem, such as sleep apnea, obesity, or medication side effects, and consequently, put you at risk of side effects like fluid retention, joint pain, insulin resistance, and abnormal tissue growth. Simply put, taking HGH as a substitute for TRT is not in line with standard clinical practice and hardly leads to the right treatment for low testosterone. Besides, it is possible to be inadvertently treated with a hormone you do not need.
Can HGH Improve Symptoms of Low Testosterone?
Sometimes, the specific hormone involved is less critical than the general sense of better training, clearer thinking, and a better sense of normalcy. That’s understandable.
The challenge is that “low testosterone symptoms” are not specific. Fatigue, lower libido, and poor recovery can come from a long list of factors. For example:
- inconsistent sleep (or breathing issues during sleep);
- under-eating, low protein intake, or rapid weight changes;
- high stress with limited downtime;
- overtraining without enough rest;
- mood conditions and medications that affect libido and energy.
This is where experience matters in a clinic setting. A clinician connects symptoms to testing, timing, and context. That helps avoid chasing one hormone label when the real issue sits somewhere else.
HGH vs Testosterone Therapy — Main Differences
Both HGH therapy and testosterone replacement therapy (TRT) are treatments that address different hormone systems, which is why they cannot be used interchangeably. HGH therapy works to increase the level of growth hormone that then leads to the production of IGF-1 and has a positive effect on tissue healing, body composition, and metabolism. Doctors usually prescribe it when a patient has been found to have growth hormone deficiency or some other type of problem with the growth hormone axis, following tests conducted by a specialist.
TRT is used to bring testosterone back to healthy levels after low testosterone has been verified through symptoms, consistent results, and repeated laboratory tests. It mainly influences sexual function, energy, mood, muscle mass, and bone density. Since testosterone can have an impact on the blood count, fertility, and prostate-related markers, it is considered normal to have follow-up tests and changes in the dosage.
In other words, in clinical settings, HGH therapy is used to treat growth hormone deficiency, whereas TRT is used to treat hypogonadism. They are different treatments for different medical conditions and involve different tests, monitoring, and expected results.
When HGH and Testosterone Are Used Together
Some patients inquire whether there are combinations to be utilized with specific combination therapy, particularly with hydrogen-structured hormone optimization programs. A solid combination discussion answers four questions:
- What diagnosis is being treated?
- What symptoms are we tracking?
- What labs need follow-up, and how often?
- What side effects or changes should trigger a reassessment?
The main purpose of combining HGH with testosterone is anti-aging. Naturally, testosterone levels and growth hormone levels decrease over a lifetime. Of course, it leads to undesired changes in energy, mood, libido, and all the above-mentioned. HGH with testosterone combination work siltamously – each medicine complements the other – genuine testosterone with the artificially produced one.
A healthcare professional may want to address more than one therapy in selected cases; however, the discussion should remain practical and measurable. Anyway, it is highly recommended to avoid self-treatment.
Risks of Expecting a Testosterone Boost From HGH
An example of a worst fear is to ignore the real reason behind your symptoms. If you are thinking HGH will solve low testosterone, you may avoid a proper evaluation that may reveal a hidden problem – maybe sleep apnea, effect from medications, or maybe there is actually a reality and low testosterone presents its own plan to be solved.
Another danger is that of inconsistency. Switching from one idea to another without any steady plan can result in a detrimental impact on your hormone balance. Hormone systems require time, routine, and a healthy overall picture to make a proper response. One-off labs and quick conclusions can lead to confusion.
This is why HGH for low testosterone can be a misleading search. The better question is: “What is causing these symptoms, and what plan matches that cause?”
Does HGH Boost Testosterone?
People often experience personal improvement through a focus on the basics that regulate much of the hormones – sleep, recovery, happy balancing, and metabolic health. If your symptoms are suggestive of low testosterone, then the next best step would be an evaluation with the help of a health care clinician, complete with repeat labs and a plan of action. Due to the fact that HGH and testosterone work differently, HGH cannot replace testosterone replacement therapy.
If you are reading this in order to find a way forward that is clearer to you, try to set a low bar: Get a baseline that you run around. Track the sleep, training, and symptoms for a couple of weeks, and then go back for repeat labs with a clinician, who will have a complete picture.
